Overview
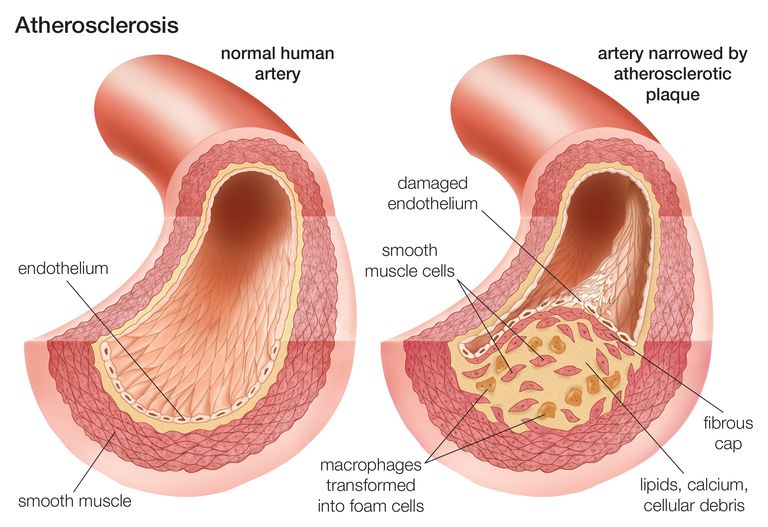
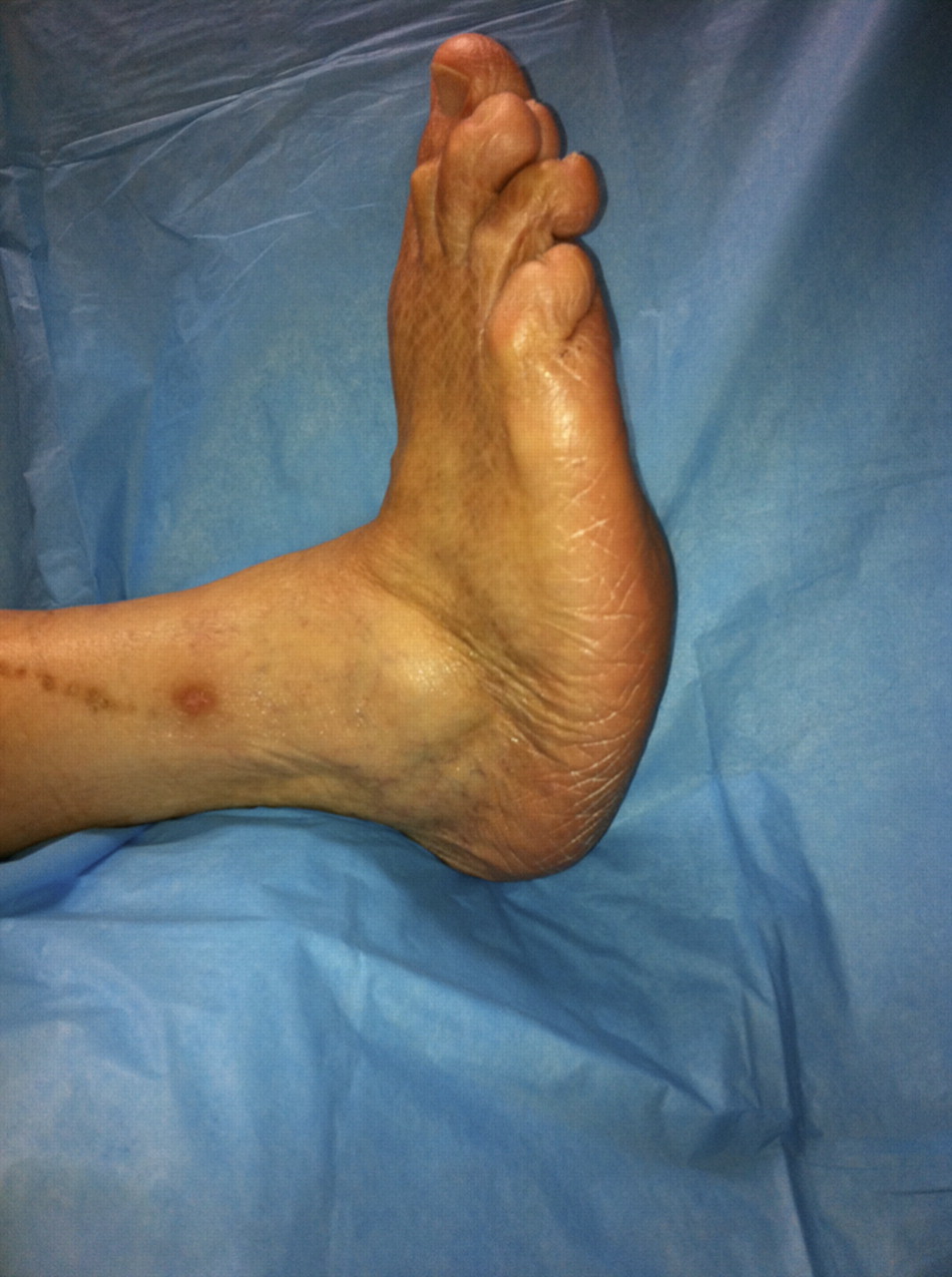
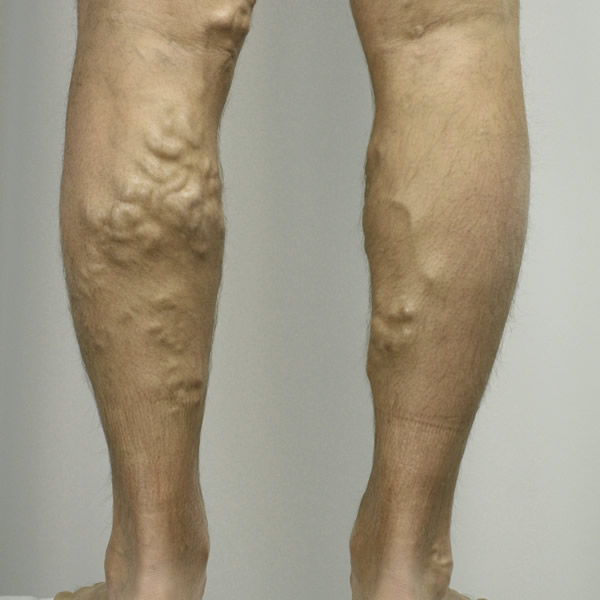
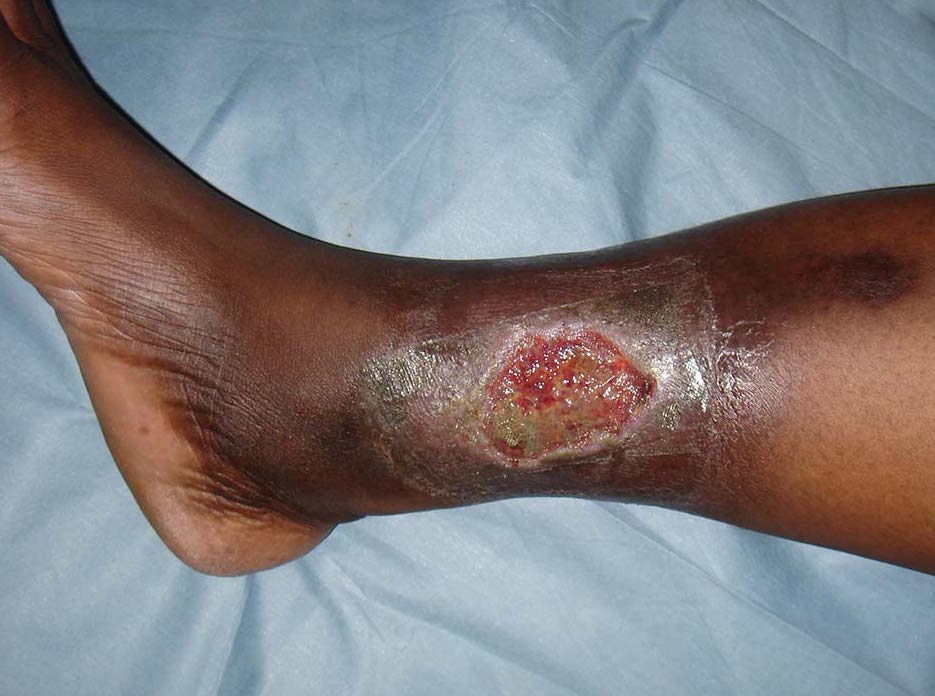
Peripheral arterial disease refers to disease affecting the arteries. This commonly affects the arteries in the legs and causes narrowing (stenosis). The reduced blood flow to the feet can manifest as a range of symptoms from: pain in the calves when exercising (claudication), pain at rest, ulceration or gangrene.
Arterial disease of the peripheries is commonly associated with risk factors such as smoking, diabetes, hypertension and high cholesterol. It is often also associated with heart disease, kidney disease and stroke.
Treatment Options.
It is essential to manage the medical risk factors aggressively. This includes measures such as stopping smoking, treating high cholesterol and blood pressure and using blood thinning agents.
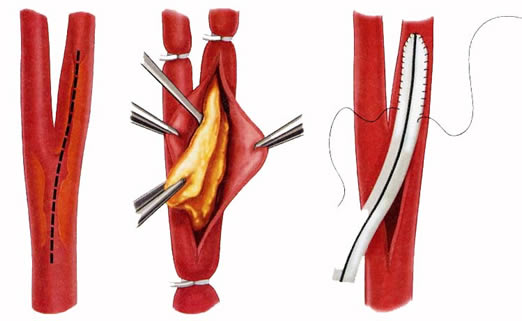
Surgical options include open surgery and minimally invasive endovascular procedures. Open surgery may include procedures such as bypass operations where a bypass conduit such as a vein is used to bypass the arterial blockage. Endovascular procedures include the use of minimally invasive techniques such as wires, balloons and stents in order to reopen the narrow or blocked artery.
Other considerations.
Different alternatives may be appropriate in differing circumstances depending on the underlying health of the patient as well as the technical aspects required for the surgery.